Order one of our free resource packs today! Fill out the form here.
University Toolkit
Hep C U Later are an NHS initiative supporting NHS England with the elimination of viral hepatitis through providing support, coordination, data analytics, engagement, resources and education to health and social care professionals across England. You can learn more about us and what we do here.
This toolkit is intended to provide a variety of options for universities to increase awareness of viral hepatitis amongst staff, students, and any organisations they collaborate with. The toolkit includes resources, training, presentations and social media posts where universities can pick which resources they would like to use depending on their own personal aims.
By using this toolkit you are playing a part in the global ambition to eliminate viral hepatitis C
Hepatitis C
Hepatitis C is a blood borne virus which left untreated can cause liver disease, cancer and death. Testing is simple, and if the virus is identified treatment is available in tablet form and more than 95% effective.
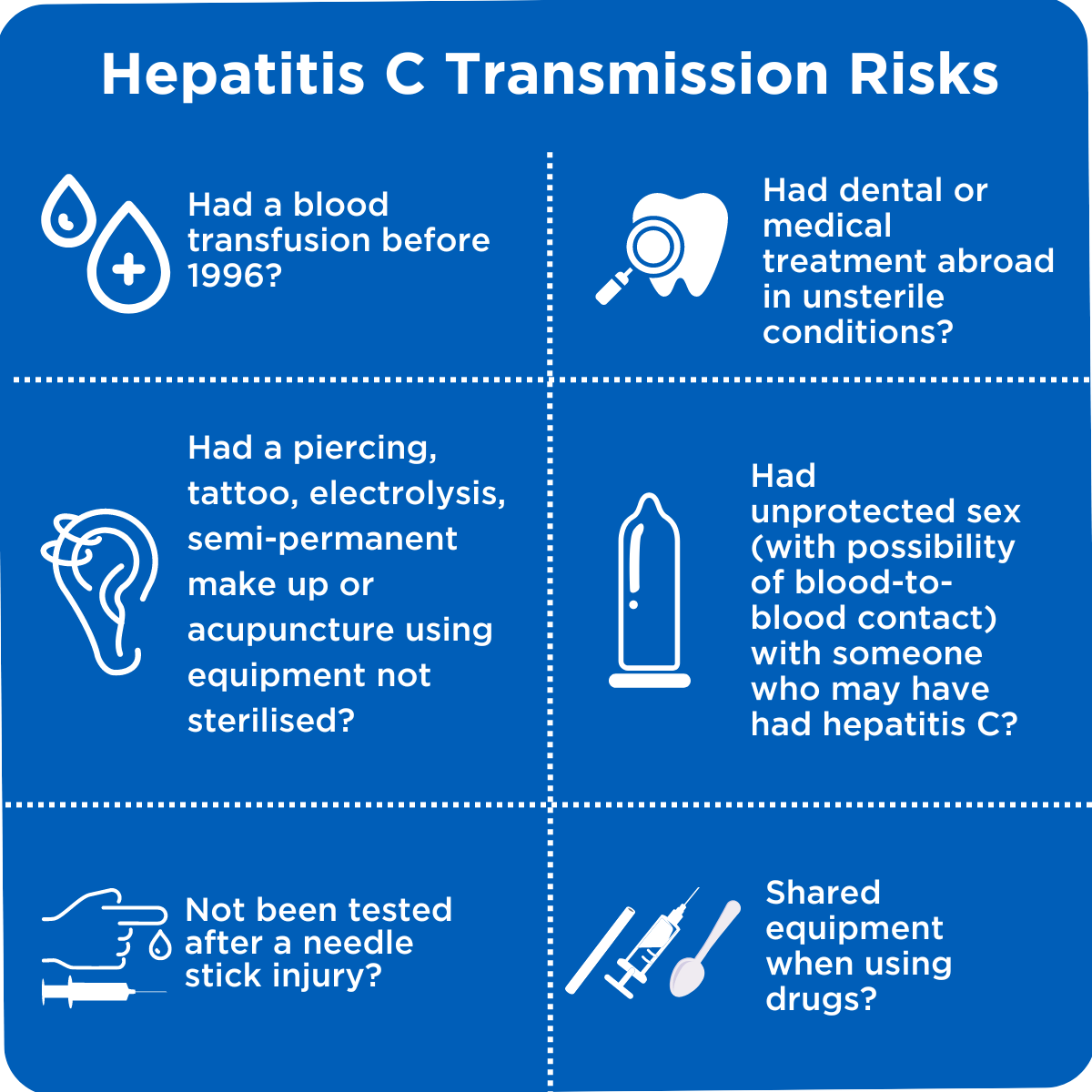
Transmission risks:
Find out more about main ways that you can come into contact with hepatitis C here.

Hepatitis C Testing
Testing is simple, and can be done through a number of ways:
- Through a GP
- Some sexual health services
- Some emergency departments offer opt-out testing
- The online hepatitis c portal, anyone in England over the age of 18 can order a free at home test for hepatitis C
Once ordered the test arrives quickly in the post. The person carrying out the test follows the instructions, collecting a blood sample in a small tube, then posts it back. If the result is positive the individual will be called to arrange treatment.
If your interesting in learning about the different forms of testing, click here.
What is Hepatitis B?
Hepatitis B is a type of viral hepatitis that affects the liver. If left untreated hepatitis B can cause liver disease, cancer and death. The virus is spread through contact with body fluids, mostly blood, from an infected person and mother to child transmission can be a common way for the virus to spread.
Most people who come into contact with hepatitis B naturally clear the virus in 6 months and then get immunity from hepatitis B following that infection (referred to as an acute hepatitis B infection). 5-10% of adults do not clear the virus naturally and require treatment to manage the virus and its effects (called a chronic infection).
Hepatitis B Risk Factors
Hepatitis B can survive outside the body for at least 7 days and is 50-100 times more infectious than HIV. It is transmitted by body fluids (vaginal and seminal), and from infected blood. Risk factors for transmission include:
- Blood transfusion prior to 1996
- Tattoos or body piercings using unsterile equipment
- Sharing equipment for injecting/preparing illicit drugs
- Needle stick injury
- Un-sterilised medical or dental equipment
- Mother to baby during delivery
- Unprotected sex with someone who has hepatitis B
Hepatitis B Testing and Results
Testing for hepatitis B is simple. Normally two tests are taken (core antibody and surface antigen) and further testing would be carried out to provide confirmation. The incubation period for hepatitis B is 40-160 days therefore, if someone thinks they have come into contact with the virus it is important to test within the correct window.
A person may get immunity to hepatitis B by either having a course of hepatitis B vaccinations, or by having the virus and the body ‘clearing’ it. Clearing the virus means that the body has fought off the infection and has produced antibodies and is referred to as ‘spontaneous clearance’.
Hepatitis B Prevention
There is a vaccine to prevent infection from hepatitis B. It is not a live vaccine meaning there is no risk of getting hepatitis B from the vaccine itself. The vaccine’s job is to trigger the immune system into recognising the virus and producing antibodies.
Some people who are alcohol dependent or who have advanced liver disease may experience a poorer immune response to the vaccine, or if a person has kidney problems/is on dialysis they may require a double dose of the vaccine. Hepatitis B vaccines are normally administered according to a ‘schedule’. Professionals administering vaccines must follow their organisation’s policies and guidance.
Hepatitis B Treatment
For most people who have a chronic hepatitis B infection antiviral treatment can be given which reduces the negative effect the virus can have on the body. The treatment aims to manage the virus rather than cure it. Hepatitis B treatment can help to prevent cirrhosis (scarring of the liver), liver failure and liver cancer by reducing the amount of virus exerting an effect on the body while improving liver enzyme levels.
Some people with low levels of the virus might not be treated but may still be monitored. Regular check-ups, blood tests and fibroscans are completed to review how the virus is progressing.

Differences between hepatitis B and hepatitis C
Key components of hepatitis B and hepatitis C can often be confusing for professionals. Here are some key differences between the two:
Hepatitis B
- Spread through blood and bodily fluids
- More commonly spontaneously cleared
- After spontaneous clearance gains immunity
- Preventative vaccine available
- No cure, however, treatment to manage infection is available
Hepatitis C
- Spread through blood to blood contact
- Less commonly spontaneously cleared
- After spontaneous clearance or curative treatment does not give immunity (can be re-infected)
- No preventative vaccine available
- Curative treatments are available

Viral Hepatitis Elimination
The World Health Organisation released the viral hepatitis elimination strategy in 2016 outlining the aim to eliminate hepatitis globally by 2030 (WHO-Global Health Sector Strategy on Viral Hepatitis 2016–2021 Towards Ending Viral Hepatitis.pdf (globalhep.org)
There are multiple examples of how services are improving the identification of hepatitis B and C, linking people to care, and improving access to treatment. Our resources pages showcase best practice case studies featuring lots of this work.
To reach the goal of viral hepatitis elimination it is essential we support students and professionals within the health and social care sector, who may come into contact with people unaware of having a viral hepatitis infection.
By spreading awareness, delivering training or encouraging people to get a test you are part of the grand global ambition of eliminating viral hepatitis as a public health threat.
Spread awareness about hepatitis C with our social media posts. Tag us and use #HepCULater

Share our free CPD Accredited Training with staff and students:
Anyone can access the free Hep C U Later CPD accredited online training.
Our training modules are for people at all levels, many modules are currently available with more being added.
Deliver a basic hepatitis C presentation within student health and social care programmes:
Hep C U Later have a presentation slide set available for university lecturers to deliver basic hepatitis C information to students. This training is particularly helpful for health and social care students to raise awareness of the national testing portal and other resources which are available. University educators can build confidence in delivering this information to students through completing the CPD accredited training mentioned above.


Handout the Hepatitis C Factsheet:
This simple hepatitis C factsheet can be sent to students on health and social care programmes alongside the CPD accredited training link or during the presentation to provide people with further information.
Visit the Hep C U Later resources and professionals pages:
The Hep C U Later website hosts multiple resources, videos, podcasts and case studies for students to use, additionally many bespoke resources can be found under the professional’s pages.

Get in touch
If you would like to know more, want something specific, or want to arrange a meeting to discuss how you can support the elimination of viral hepatitis email us – connect.HepCULater@mpft.nhs.uk